Because Every Tooth Deserves Care.
Why Bone Grafts Fail in Some Dental Clinics: Risks, Causes, and Patient Advice
Language :

Topics:
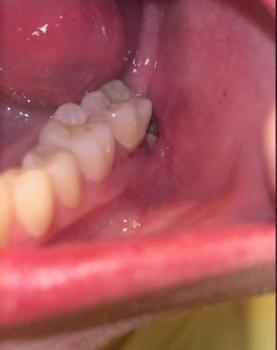
Bone grafting is a common procedure used in implant dentistry to rebuild jawbone that has been lost due to tooth extraction, gum disease, or trauma. A successful bone graft creates enough bone volume to support a dental implant securely.
However, in some cases bone grafts fail. Patients may experience infection, poor bone formation, or graft rejection. One concern sometimes discussed in dental communities is that some clinics may perform bone graft procedures even when the patient is not an ideal candidate, often because the procedure is profitable.
Understanding why bone grafts fail helps patients make informed decisions and choose experienced dental professionals.
What Is a Dental Bone Graft?
A bone graft is a surgical procedure used to replace or regenerate missing bone in the jaw.
Dentists may recommend bone grafting when:
• The jawbone is too thin for dental implants
• Bone has shrunk after tooth loss
• Severe gum disease has damaged bone
• Trauma or infection caused bone loss
The graft material acts as a scaffold that allows new bone to grow and integrate with the patient’s natural bone.
Do I need bone graft for implant," "jawbone healing after tooth loss" ?
Common bone graft materials include:
• Autograft (patient’s own bone)
• Allograft (donor bone)
• Xenograft (animal-derived bone)
• Synthetic bone substitutes
Healing typically takes 3 to 6 months before implants can be placed.
Why Bone Grafts Sometimes Fail
Bone graft failure is not extremely common, but it can occur for several reasons.
1. Poor Patient Selection
One major cause is improper case selection.
Not every patient is an ideal candidate for bone grafting. Certain health conditions reduce the body’s ability to regenerate bone.
Risk factors include:
• Uncontrolled diabetes
• Heavy smoking
• Severe gum disease
• Poor oral hygiene
• Weak immune system
If these conditions are not properly managed before surgery, graft failure becomes more likely.
In some situations, financial pressure or aggressive treatment planning may lead a clinic to recommend procedures even when success chances are low.
2. Infection After Surgery
Infection is one of the most common causes of bone graft failure.
Bacteria can contaminate the surgical site if:
• Sterilization protocols are inadequate
• The patient does not follow post-operative care instructions
• Existing oral infections were not fully treated before surgery
An infected graft may not integrate with the natural bone, leading to failure.
3. Poor Surgical Technique
Bone grafting requires precise surgical technique.
Potential issues include:
• Incorrect graft placement
• Insufficient stabilization of the graft material
• Damage to surrounding tissue
• Poor blood supply to the graft area
If the graft does not receive adequate blood supply, new bone cannot develop properly.
4. Lack of Bone Integration
For a graft to succeed, the body must create new bone cells that merge with the graft material.
Failure can occur if:
• The graft material does not integrate
• The body rejects the material
• The healing environment is not stable
Movement in the graft area can also prevent proper bone formation.
5. Smoking and Lifestyle Factors
Smoking significantly increases the risk of graft failure.
Nicotine reduces blood flow and interferes with bone healing. Smokers often experience slower healing and higher complication rates after oral surgery.
Other lifestyle factors that affect bone graft success include:
• Poor nutrition
• Excess alcohol consumption
• Chronic stress
• Poor oral hygiene
Financial Pressure and Ethical Concerns
Some patients worry that certain clinics recommend bone grafting primarily because it increases treatment costs.
Dental implants often require supporting procedures such as:
• Bone grafts
• Sinus lifts
• Guided bone regeneration
These procedures add significant cost to treatment plans.
Ethical dentists carefully evaluate whether bone grafting is truly necessary. In some cases, alternative treatments may be more appropriate.
Examples include:
• Short dental implants
• Mini implants
• Implant placement in stronger bone areas
• Bridge restorations
Patients should always seek clear explanations and second opinions when treatment plans involve multiple surgical procedures.
Signs That a Bone Graft May Be Failing
Early detection of problems is important.
Possible warning signs include:
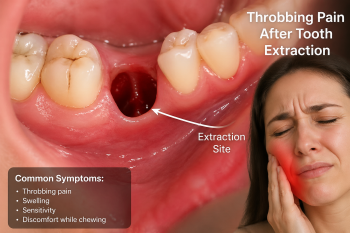
• Persistent swelling or pain
• Gum infection near the graft site
• Pus or unusual discharge
• Exposure of graft material
• Implant instability after placement
If any of these symptoms occur, patients should contact their dentist immediately.
Prompt treatment may prevent further complications.
How to Reduce the Risk of Bone Graft Failure
Patients can improve success rates by following several important guidelines.
Choose an Experienced Implant Dentist
Experience plays a major role in surgical success. Dentists who specialize in implant surgery often perform advanced diagnostic imaging and treatment planning before recommending bone grafting.
Proper Pre-Surgical Evaluation
A thorough examination should include:
• 3D CBCT imaging
• Bone density analysis
• Review of medical history
• Evaluation of gum health
These steps help determine whether bone grafting is appropriate.
Stop Smoking Before Surgery
Patients who smoke are strongly advised to stop smoking several weeks before and after surgery. This significantly improves healing.
Follow Post-Operative Instructions
Proper care after surgery is critical. Patients should follow instructions regarding:
• Oral hygiene
• Antibiotic use
• Diet restrictions
• Avoiding pressure on the surgical site
Alternatives to Bone Grafting
In some cases, modern implant techniques can avoid the need for bone grafting.
These options may include:
All-on-4 Dental Implants
This technique uses angled implants to anchor teeth in stronger areas of bone, often avoiding the need for grafts.
Zygomatic Implants
These specialized implants anchor into the cheekbone instead of the jawbone, providing support even when jawbone volume is very limited.
Short Implants
Advances in implant design allow shorter implants to function successfully in thinner bone.
These alternatives can reduce treatment time and avoid additional surgical procedures.
The Importance of Honest Treatment Planning
Good dentistry focuses on long-term patient outcomes rather than unnecessary procedures.
Responsible dentists evaluate whether bone grafting will truly benefit the patient. When the chances of success are low, they may recommend alternative treatment options.
Patients should feel comfortable asking questions such as:
• Why is bone grafting necessary?
• What are the success rates?
• Are there alternative treatments?
• What are the total treatment costs?
Transparency helps build trust between dentists and patients.
Conclusion
Bone grafting plays an important role in modern implant dentistry, allowing many patients to restore missing teeth even after bone loss.
However, bone grafts can fail if the patient is not a suitable candidate, if infection occurs, or if surgical technique is inadequate. Lifestyle factors such as smoking and poor oral hygiene also increase the risk of complications.
Patients should carefully research dental clinics, ask questions about treatment plans, and consider second opinions when complex procedures are recommended.
Choosing experienced dental professionals and maintaining good oral health habits greatly improves the chances of successful bone graft and dental implant treatment.
Related Topics
- Why Dental Implants Fail in Some Clinics
- All-on-4 Dental Implants vs Traditional Implants
- How Long Do Dental Implants Last
- Bone Grafting for Dental Implants: What Patients Should Know
- Dental Implant Infection: Causes and Prevention
FAQ:
Common Causes of Bone Graft Failure
Bone graft failure can happen due to several factors related to patient behavior, health conditions, or surgical complications. One common cause is post-surgery mistakes, such as smoking, poor oral hygiene, touching the surgical area, or eating hard foods too soon. These actions can disturb the graft and prevent proper healing.
Smoking is a major risk factor because nicotine reduces blood flow to the gums and jawbone, limiting the oxygen and nutrients needed for bone regeneration. Infection is another serious issue; symptoms may include swelling, pain, pus, or gum redness. If infection occurs, the graft may need to be removed before another attempt can be made.
Patients with certain medical conditions—such as uncontrolled diabetes, severe gum disease, or immune disorders—may also have a higher risk of graft failure. In some cases, dentists may recommend bone grafts even when alternatives exist, so patients are encouraged to ask questions or seek a second opinion.
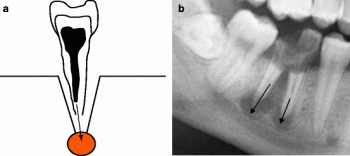
Signs of graft failure may include persistent pain, swelling, exposed graft material, or implant instability. Dentists often confirm problems through X-rays or 3D scans. If a graft fails, another graft procedure or alternative implant techniques—such as All-on-4 implants, zygomatic implants, or short implants—may be considered.
Patients can improve success rates by choosing an experienced implant dentist, maintaining good oral hygiene, avoiding smoking, and following all post-surgery instructions carefully.
Can tooth extraction cause infection? Mild inflammation is normal, but increasing swelling, fever, or severe pain may indicate infection. Learn more about post-extraction infection warning signs in this detailed guide.
Book a consultation with our Cebu dental specialists for proper evaluation and care.
Ready to get expert guidance?
If you’re experiencing severe pain or delayed healing, book a consultation with our Cebu dental specialists to get proper evaluation and care.
Consultation or contact page .
Book a Consultation
For severe discomfort or delayed healing, book a consultation with our Cebu dental specialists today.
Looking for a dentist? Browse our Cebu dental directory to find trusted clinics near you.
Medical Review and Clinical Basis
This article is based on clinical dental guidelines and real patient recovery patterns observed after tooth extraction procedures. The information reflects common post-extraction healing stages, including normal clot formation, gum tissue repair, and signs of possible complications such as dry socket or infection.
While mild discomfort is expected after a dental extraction, worsening pain after Day 3, bad odor, exposed bone, or spreading pain may require professional evaluation. These symptoms are consistent with known post-extraction complications described in standard dental practice.
About Cebu Dental Implants
Cebu Dental Implants provides comprehensive tooth extraction, surgical procedures, and dental implant services in the Philippines. Our team evaluates post-extraction healing, manages complications such as dry socket, and advises patients on proper aftercare to prevent infection and delayed healing.
If you experience severe pain or unusual symptoms after extraction, early professional assessment is recommended to prevent further complications.
Important Medical Disclaimer
This content is for educational purposes only and does not replace professional dental diagnosis. Every patient heals differently. If symptoms worsen or do not improve within a few days, consult a licensed dentist for proper evaluation and treatment.
Author
This article was prepared by the Cebu Dental Implants content team in consultation with licensed dental professionals experienced in tooth extraction and implant procedures.