Dentures That Feel Natural, Look Beautiful.
From Abscess to Anatomy: Understanding Maxillary Molar Pathology and Surgical Planning
Language :
Topics:
1. Case Analysis: Diagnosis and Urgent Management
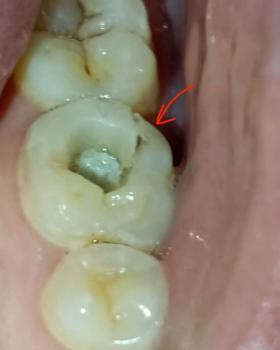
The uploaded image shows a severe infection originating from the upper right posterior segment (maxillary arch).
| Feature Observed | Significance and Diagnosis |
| Severely Decayed Molar | The most posterior tooth visible is non-restorable, having deep caries (decay) that has penetrated the pulp, causing pulp necrosis (nerve death) and acting as the source of infection. |
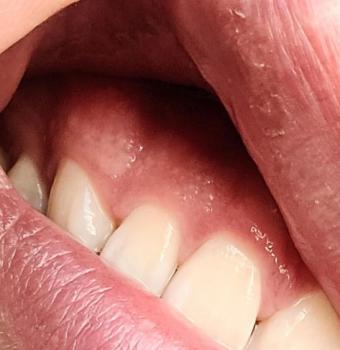
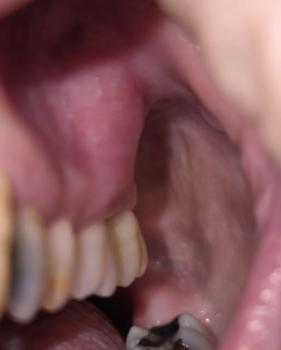
| Palatal Swelling/Bulge | A distinct, localized swelling is present on the Hard Palate adjacent to the decayed tooth. This is a classic sign of a Periapical Abscess—a collection of pus at the root tip—that has found a path of least resistance through the bone and is forming a fistula (a draining tract) on the palate. |
| Client History | Bleeding and inability to perform extraction due to low sinus floor. This confirms the infection is chronic, has destroyed bone, and now poses a risk to the Maxillary Sinus. |
| Medication | Amoxicillin 500mg Q8H (every 8 hours) is necessary to contain the acute bacterial spread prior to definitive surgical treatment. |
The Primary Diagnosis: Chronic Maxillary Periapical Abscess associated with severe tooth decay, complicated by proximity to a low Maxillary Sinus floor.
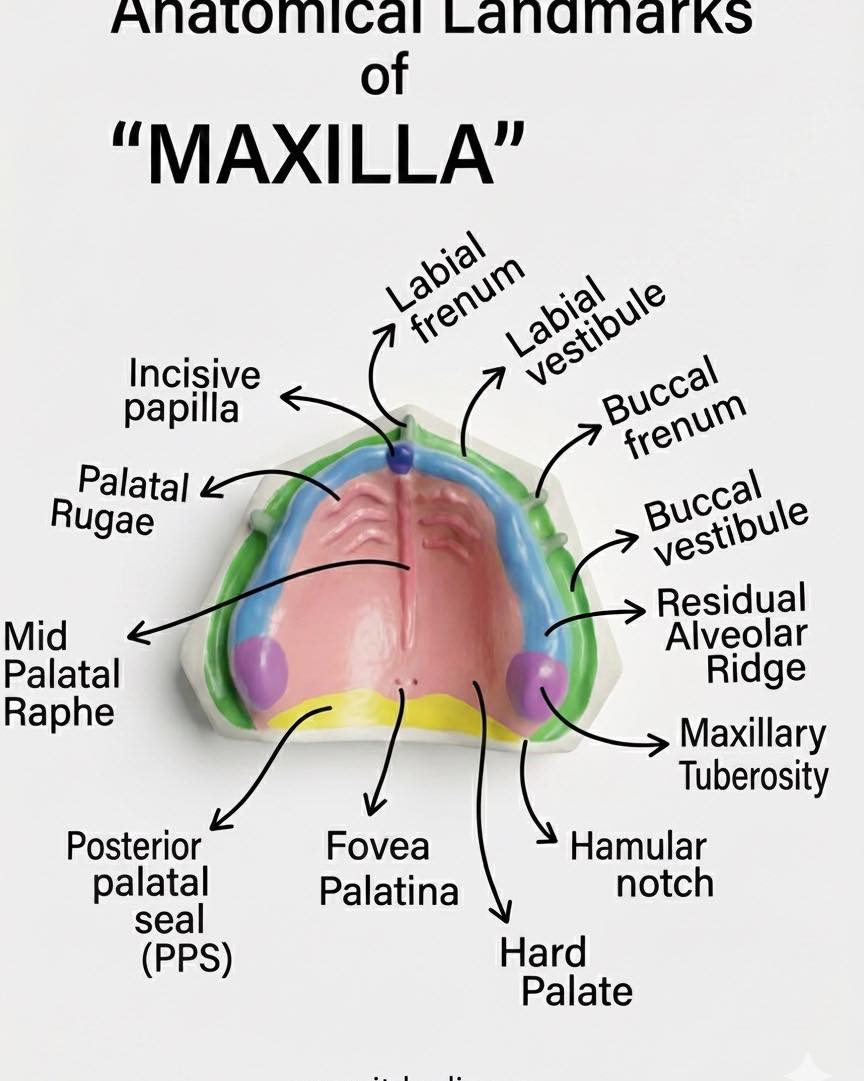
2. Anatomical Landmarks of the Maxilla: A Student's Guide
Understanding the maxilla's landmarks (as shown in the second image) is crucial for appreciating the risk in this case. The infection is situated within the Alveolar Process (the part of the maxilla that holds the teeth).
The table below enumerates and compares the functions of the key landmarks that a dental professional interacts with.
| Landmark Name | Function/Location | Clinical Relevance (Comparison) |
| Hard Palate | Forms the roof of the mouth and the floor of the nasal cavity. It is composed of the palatine processes of the maxilla and the horizontal plates of the palatine bone. | The Palatal Swelling in the case sits directly on this landmark. Bone is thicker here than on the buccal (cheek) side, indicating a more aggressive infection path. |
| Alveolar Ridge/Process | The thickened bone structure that contains the tooth sockets (alveoli). It rapidly remodels (resorbs) after tooth extraction. | Location of the Pathology. This area is compromised by infection-driven bone loss and is the target site for the surgical extraction and necessary bone grafting. |
| Maxillary Tuberosity | The rounded, distal prominence of the alveolar process located behind the last molar. It is a dense area for denture support. | Surgical Endpoint. A fixed point for posterior surgical planning, ensuring adequate bone remains distally after the extraction of the problematic molar. |
| Mid Palatal Raphe | A prominent ridge running down the midline of the Hard Palate. Represents the fusion line of the palatine shelves during development. | Anesthesia & Implant Placement. Used as a central reference point. Its dense nature makes it a difficult area for injections or placing certain implants (e.g., palatal expanders). |
| Incisive Papilla | A small pad of tissue behind the upper central incisors, covering the opening of the incisive canal (transmitting the nasopalatine nerve/vessels). | Nerve Block. This landmark serves as a reference point for the infiltration of the nasopalatine nerve block, which is essential for anesthetizing the palatal tissues in the anterior region. |
3. Surgical Implications: Process to Execute
The primary issue is the proximity of the molar root tips to the Maxillary Sinus floor. Long-standing infection has likely destroyed the thin layer of bone separating the root tip from the sinus cavity.
Process to Execute (Surgical Plan for the 24th)
-
Infection Control: Confirm infection is stable (Amoxicillin).
-
Surgical Extraction: The oral surgeon must remove the tooth atraumatically (gently) to prevent tearing the sinus lining (Schneiderian Membrane).
-
Oro-Antral Communication (OAC) Check: The socket will be inspected. If a hole exists (OAC), it must be immediately sealed.
-
Sinus Floor Elevation/Grafting: A procedure known as a Sinus Lift may be performed concurrently or planned for the future. The OAC is sealed, and bone graft material is placed to regenerate the bone lost to infection and prepare the site for a potential future implant.
Time Frame to Heal
-
Initial Recovery: 7–14 days for the soft tissues (gums) to close and the acute pain/swelling to resolve. The patient will be placed on strict post-operative instructions (e.g., no nose blowing, no straws).
-
Bone Healing: If a bone graft (Sinus Lift) is performed, it requires 3 to 6 months to fully mature and integrate before the site is stable enough for a dental implant.
Conclusion and Next Step
The patient is in the critical phase of antibiotic coverage and is scheduled for the definitive treatment. The Oral and Maxillofacial Surgeon is essential to safely remove the tooth, eliminate the infection, and manage the anatomical complication of the low sinus floor and potential OAC.