Your Smile, Perfected with Precision.
Surgical Closure of Oro-Antral Communication (OAC): Techniques and Post-Operative Imperatives
Language :

Topics:
The Surgeon's Arsenal: A Guide to Essential Dental Extraction Instruments
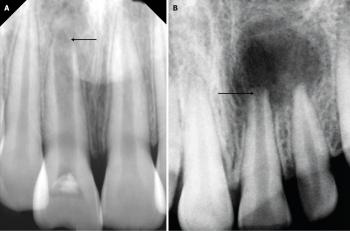
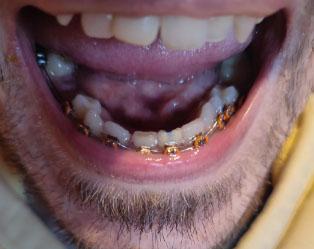
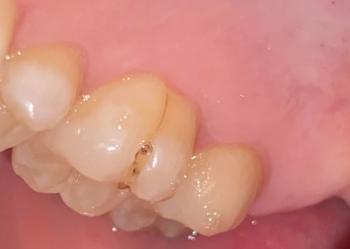
The success of any dental procedure, especially complex surgery like the extraction required for the severe periapical abscess case shown, depends on the precision and function of its instruments. This post provides a detailed breakdown of the instruments found in a typical surgical/extraction kit, visible in the provided image.
1. Diagnostic and Auxiliary Instruments
These instruments are used for initial examination, manipulation of soft tissues, and general procedure assistance. They are typically found in the upper left section of the kit.
| Instrument Name | Function | How to Use |
| Mouth Mirror | Used to reflect light, provide indirect vision, and retract the cheek or tongue for better access. | Held in the non-dominant hand. Essential for checking posterior or lingual (tongue side) surfaces. |
| Explorer | A sharp, pointed instrument used to detect dental caries (decay), check the margin integrity of restorations, and examine the texture of the tooth surface. | Held with a modified pen grasp. The tip is drawn lightly across the tooth surface; a "catch" or resistance indicates a carious lesion. |
| Periapical Curette (or Surgical Spoon Excavator) | A double-ended spoon-shaped tool used to scoop out soft tissue, debris, granulation tissue, or infected material (like an abscess) from the tooth socket or surgical site. | Used after extraction. Inserted into the socket or bony defect and gently scraped against the walls to remove pathology. |
| Cotton Pliers/Forceps | Tweezer-like instruments used to grasp and transfer small items (like cotton pellets, gauze, or paper points) into and out of the mouth. | Held like chopsticks. Used to maintain a sterile transfer of materials. |
| Retractors (Various) | Used to hold the lip, cheek, or tongue away from the operating field to maintain visibility and prevent injury. | Held in the assistant's hand or secured by the surgeon, applying gentle, steady pressure to tissue. |
| Surgical Scissors | Used to cut soft tissue (gums), sutures, or to trim surgical dressings. | Used with a finger grasp. Held like standard scissors, ensuring only tissue or suture material is cut, never bone. |
2. Anesthesia and Soft Tissue Management
These tools are crucial for achieving profound numbness and managing the gum tissue prior to tooth removal.
| Instrument Name | Function | How to Use |
| Aspirating Syringe | Used to administer local anesthesia. It allows the clinician to aspirate (pull back on the plunger) to ensure the anesthetic is not injected directly into a blood vessel. | Loaded with an anesthetic cartridge and needle. Before injection, the plunger is pulled to check for blood return; if clear, the injection proceeds slowly. |
| Scalpel Handle (e.g., Bard-Parker Handle) | Used to hold various scalpel blades (like a #15C or #12) for making precise surgical incisions in the gingiva and mucous membrane. | A sterile blade is locked onto the handle. Used to create a flap (an incision in the gum) for surgical access to the tooth and bone. |
| Periosteal Elevator | Has a sharp, rounded end and a flat, blunt end. Used to reflect (lift) the gingiva and the underlying periosteum (connective tissue covering the bone) off the alveolar bone. | The sharp end is used to initiate the lift, and the blunt end is used to push the tissue cleanly away from the bone, exposing the surgical site. |
3. Extraction Instruments: The Core Arsenal
This is the main group of instruments used for the actual tooth removal process, visible in the right and bottom sections of the kit.
A. Elevators
Elevators are used to luxate (loosen) the tooth from the socket, expand the bony socket walls, and aid in the removal of fractured roots.
| Instrument Name | Function | How to Use |
| Straight Elevator (e.g., #301, #34S) | Used to apply force (wedge, lever, or wheel-and-axle principle) into the periodontal ligament space to loosen the tooth before forceps application. | Inserted into the PDL space and rotated or wedged against the tooth and bone to slowly expand the socket and lift the tooth. |
| Apex Elevator (or Root Tip Pick) | Very small, thin-tipped elevators used specifically to remove fractured or retained small root tips from the socket. | Inserted into the socket alongside the root fragment, using minimal force to gently tease the root tip out. |
| Cryer Elevator | Paired (left and right) with triangular-shaped tips. Used specifically for removing broken root fragments, often by rotating the tip into the empty socket of the adjacent root. | Used as a wheel-and-axle to engage and lift a retained root segment. |
B. Extraction Forceps
Forceps are used to grasp the tooth firmly, apply controlled forces (buccal-lingual/rocking motion, rotation, and traction) to further break down the periodontal ligament, and deliver (pull) the tooth from the socket. Each type is uniquely shaped to fit the anatomy of a specific tooth (e.g., single root, three roots).
| Instrument Name | Function | How to Use |
| Maxillary Universal Forceps (e.g., #150) | Designed for upper (maxillary) anterior and premolar teeth. The beaks are straight and the handle is offset. | The beaks grasp the neck of the tooth; controlled force is applied in a bucco-lingual (outward-inward) motion to luxate and remove the tooth. |
| Maxillary Molar Forceps (e.g., #53L, #53R, or #88 "Cowhorn") | Specifically shaped with a point or cusp on one beak to fit into the buccal trifurcation (where the three roots meet) of upper molars. | Used to engage the roots deeply. Rocking motion applied carefully to avoid fracturing the fragile sinus floor bone, especially in a case like the one shown. |
| Mandibular Universal Forceps (e.g., #151) | Designed for lower (mandibular) anterior and premolar teeth. The beaks are angled differently to allow access to the lower arch. | Used with a rocking motion, primarily mesial-distal (front-back), as the bone is denser than the maxilla. |
| Mandibular Molar Forceps (e.g., #23 "Cowhorn") | Has two sharp points (horns) on both beaks that fit into the buccal and lingual bifurcations of lower molars. | Used to stabilize the tooth by grasping the roots directly, minimizing crushing of the crown. |
4. Suturing and Hemostasis
These instruments are used to close the surgical site and control bleeding.
| Instrument Name | Function | How to Use |
| Needle Holder | Used to securely grasp and control the surgical needle during the placement of sutures (stitches) to close the incision or socket. | Held with a finger lock. The needle is grasped near the middle, and the needle holder guides the needle through the tissue. |
| Tissue Forceps (often Adson's) | Tweezer-like instruments with small teeth used to gently grasp and stabilize soft tissue (like the gum flap) while placing sutures. | Held like cotton pliers, used to steady the tissue to ensure the needle passes through accurately. |
By mastering the function and proper application of each of these instruments, dental students can confidently approach surgical extractions and manage complex anatomical scenarios like the maxillary molar abscess shown in the case study.
Surgical Management: Sealing the Maxillary Sinus
An OAC is a direct communication between the alveolar process (mouth) and the maxillary sinus (nasal cavity). If left unsealed, it can lead to chronic sinusitis and persistent infection.
1. Assessment: Confirming the OAC
The surgeon must first confirm if the sinus lining (Schneiderian Membrane) has been breached.
-
Extraction: The compromised molar is removed gently using specialized forceps (like the Maxillary Molar Forceps) and elevators to minimize bone trauma. The infected tissue (abscess) is then thoroughly curetted (scooped out) from the socket.
-
The Nasal Blow Test: The most common diagnostic test. The surgeon asks the patient to gently pinch their nose shut and blow.
-
Positive Result: Air or bubbles pass into the mouth through the socket. This confirms the presence of an OAC.
-
Negative Result: No air passes, suggesting the membrane is either intact or the OAC is very small.
-
2. Treatment Options: Sealing the Defect
The size and chronicity of the OAC determine the closure technique. Given your history of a low sinus floor and chronic infection, a significant closure procedure is often necessary.
A. Primary Closure (The Buccal Flap Technique)
This is the most common technique used for fresh OACs (less than 48 hours old or those that happen during the procedure).
-
Tissue Mobilization: A surgical flap (a section of gum tissue) is created on the buccal (cheek) side. The periosteum (the tissue lining the bone) is partially cut, allowing the flap to be stretched over the defect without tension.
-
Repositioning and Sealing: The stretched buccal flap is brought palatally (towards the roof of the mouth) to completely cover the open socket and overlap the edges of the bone defect.
-
Suturing: The flap is meticulously stitched (sutured) shut using non-resorbable or slowly resorbable sutures to create a watertight seal. This is crucial for preventing infection and ensuring proper healing.
B. Palatal Flap Technique (Less Common, for Larger Defects)
For very large or chronic defects, a flap from the dense Hard Palate may be mobilized. While this provides thicker, more reliable tissue, it leaves a secondary wound site on the palate.
C. Sinus Lift and Grafting (If Future Implant is Planned)
If the patient desires a future dental implant (a common goal for a missing molar), the surgeon may perform a Sinus Floor Elevation (Sinus Lift) concurrently:
-
Membrane Repair: The Schneiderian membrane is carefully separated from the sinus floor and any tears are repaired.
-
Bone Grafting: Bone substitute material (graft) is gently placed between the membrane and the sinus floor.
-
Closure: The socket is sealed with a collagen membrane and/or a primary closure (Buccal Flap) to protect the graft and prevent contamination.
3. Post-Operative Instructions: Critical for Success
The success of the closure depends almost entirely on the patient's adherence to post-operative care, which aims to maintain negative pressure in the mouth and prevent positive pressure in the nasal cavity.
| Action | Why It's Forbidden |
| Blowing the Nose | Creates high pressure in the sinus, which could immediately tear the delicate surgical sutures and re-open the OAC. |
| Sucking on Straws | Creates strong negative pressure in the mouth, which can dislodge the blood clot and pull the healing tissue apart. |
| Violent Spitting | Creates negative pressure, risking the breakdown of the closure site. |
| Smoking | The sucking motion dislodges the clot, and the heat/chemicals severely impair healing and increase infection risk. |
| Violent Sneezing | Can be unavoidable, but the patient is instructed to sneeze with their mouth open to equalize pressure and protect the surgical site. |
The surgeon will also prescribe antibiotics and often a nasal spray/decongestant to help keep the sinus clear and reduce the pressure from the inside, significantly aiding the healing process.