Transforming Smiles, Restoring Confidence.
Occlusal fracture / caries - urgent assessment and temporary protection recommended
Severity:
Teeth Problems:
Quick clinical impression
-
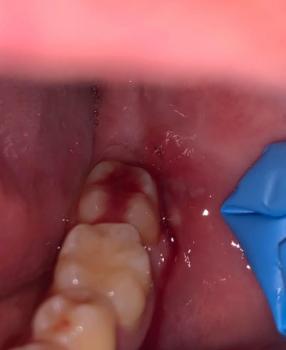
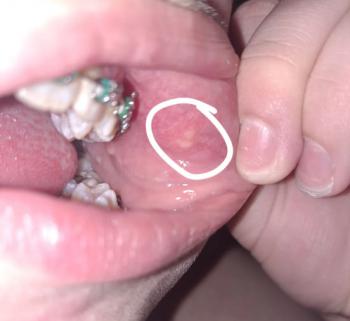
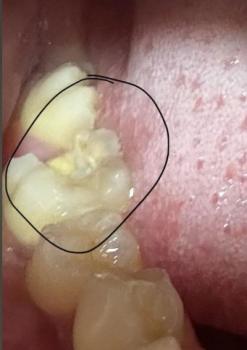
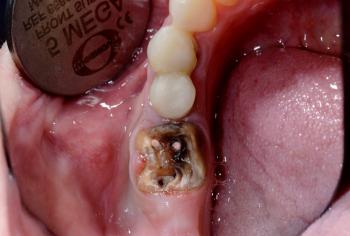
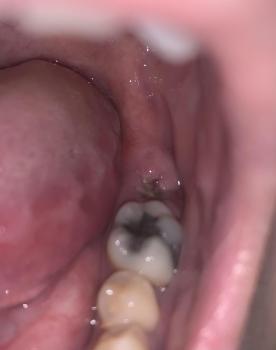
The picture shows occlusal breakdown / possible caries or fractured cusp on the last visible molar (upper right in the photo). The tooth surface looks cavitated and stained; one area looks like loss of enamel/restoration.
-
I don’t see obvious swelling or pus in the photo, and I can’t test percussion/mobility or pulp vitality from a photo — those are needed for definitive diagnosis.
-
Plain summary: likely broken tooth and/or occlusal caries — possibly exposing dentine (explains the “matulis”/sharp feeling).
Your question: “Need ko na ba ng pasta asap?”
If by “pasta” you mean a temporary filling / dental cement to cover the sharp/broken area — yes, it’s reasonable to get the tooth temporarily covered as soon as possible to:
-
stop the sharp edge from cutting your tongue/cheek,
-
reduce sensitivity and bacterial ingress,
-
lower the chance of acute pulpitis or infection.
Best option is to have a dentist place a proper temporary restoration (or definitive restoration) at an urgent visit. There are OTC temporary filling kits (dental cement/temporary cement) that can be used short-term, but they’re a stopgap — see a dentist within a few days.
Is urgent care required now or can it wait?
-
Urgent (see dentist within 24–72 hours) if you have: severe pain, swelling, fever, spreading facial swelling, pus, or increasing throbbing pain.
-
Priority within a few days if you have sharp edges, persistent sensitivity to cold/hot/sweet, or pain when biting.
-
If only mild sensitivity and no swelling, you can book an appointment soon — but don’t delay weeks if the tooth is sharp or painful.
What the dentist will do / treatment options
-
Clinical exam + bitewing/periapical X-ray to assess depth of decay and proximity to pulp and bone.
-
If shallow caries / fracture: clean and place a permanent composite filling or onlay/inlay.
-
If deep caries with pulp involvement: root canal treatment (endodontic) then crown or large filling.
-
If unrestorable or severely fractured: extraction and replacement options (bridge, implant) discussed.
-
If temporary protection needed same day: dentist may place a temporary cement or glass ionomer to cover the area.
Pain control & medicines while breastfeeding (important)
-
Paracetamol (acetaminophen): safe while breastfeeding.
-
Ibuprofen: generally safe and preferred for dental pain/inflammation while breastfeeding.
-
Local anaesthetic (lidocaine) used for dental work: safe for breastfeeding — do NOT stop breastfeeding for local anaesthesia.
-
Antibiotics if needed: amoxicillin and metronidazole are commonly used and generally compatible with breastfeeding. Avoid tetracyclines. Your dentist will choose an appropriate antibiotic if there is infection.
-
Avoid strong opioids unless absolutely necessary — discuss with provider.
If you only have 14 days — what to expect
-
Within 14 days: with temporary protection and good care, you may avoid acute infection and reduce discomfort. However if decay or fracture is deep, pulpitis or abscess can develop within days to weeks.
-
If left untreated for 14 days and the pulp is already inflamed/exposed, you may progress to more intense pain, swelling, or infection requiring root canal or extraction.
What will scale up (risks) if you wait
-
Pulp infection → irreversible pulpitis → root canal or extraction.
-
Acute dental abscess with swelling and systemic symptoms.
-
Spread of decay to adjacent teeth.
-
Bite problems or further cusp fracture, increasing restorative complexity and cost.
Immediate self-care you can do today
-
Avoid chewing on that side; stick to soft foods.
-
Salt-water rinses (warm saline) 1–2× daily if irritated.
-
Cover sharp edge temporarily: dental wax (orthodontic wax) or a dab of sugar-free chewing gum can blunt the sharp edge until you see the dentist. OTC temporary filling kits exist (follow instructions).
-
Use desensitizing toothpaste and avoid very hot/cold foods if sensitive.
-
Pain meds: paracetamol or ibuprofen as needed (follow dose instructions). Safe while breastfeeding.
-
Book an appointment — use your directory: https://cebudentalimplants.com/map-dental-clinic
Practical timeline for treatment
-
Same day/urgent (0–3 days): temporary cover or emergency visit if severe pain/swelling.
-
Within 1–2 weeks: definitive restorative treatment (filling, onlay), or endo assessment if deep.
-
If endo needed: root canal usually completed in 1–2 visits over 1–3 weeks, then final restoration (crown) in subsequent weeks.